That persistent, throbbing toothache is more than just an annoyance. It's often the first and most obvious warning sign that you might have a dental infection. This isn't the kind of minor sensitivity you get from cold drinks; it's a significant, deep pain telling you that bacteria may have gotten past your tooth's defenses.
When this happens, professional dental care is crucial to get things back on track. At Trinity Dental Care, we believe patient education is the first step toward a healthy, lasting smile.
Understanding the First Warnings of a Tooth Infection
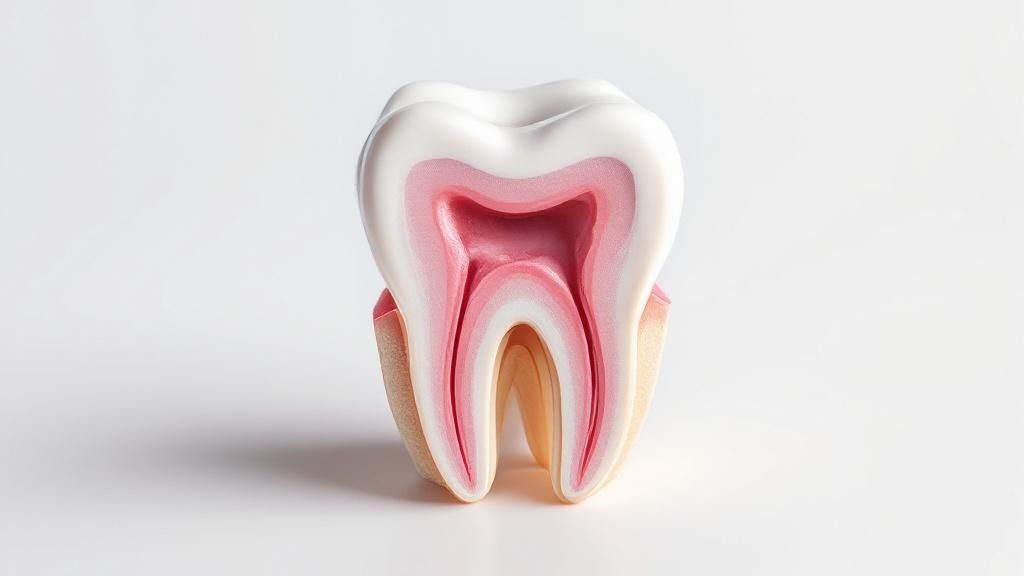
Think of a tooth infection as your body’s built-in alarm system. It goes off when harmful bacteria manage to sneak into the sensitive, inner layers of a tooth, usually through an untreated cavity, a crack, or an old injury. Ignoring these early warnings is a gamble with your health, as a seemingly small problem can escalate much faster than you’d think.
When bacteria reach the pulp—the very core of the tooth that houses all the nerves and blood vessels—the body’s natural inflammatory response kicks in. This is what causes the classic, unmistakable symptoms of an infection.
Key Symptoms to Monitor
Your body is skilled at letting you know when an infection is brewing. Paying close attention to these signals is the first step toward protecting not just your oral health, but your overall well-being. To help you know what to look for, we've put together a quick guide summarizing the common red flags.
Quick Guide to Dental Infection Symptoms
| Symptom | What It Feels Like | Potential Meaning |
|---|---|---|
| Persistent, Throbbing Pain | A severe, constant ache or sharp, shooting pain that won't go away. | This is the classic sign of inflammation inside the tooth's pulp. |
| Swelling and Redness | Noticeable puffiness in the gums, cheek, or jaw around the sore tooth. | A clear indicator that the infection is active and spreading. |
| Foul Taste or Odor | An unpleasant, metallic, or bitter taste, or bad breath that brushing doesn't fix. | An abscess may be releasing pus into your mouth. |
| Fever | Feeling unwell and developing a low-grade or high fever. | A serious sign that the infection is spreading beyond the tooth. |
These symptoms often point to a dental abscess, which is a pocket of pus that forms at the root of the infected tooth. An abscess will not go away on its own; it requires professional treatment to resolve.
For many patients in this situation, a root canal is the best path forward. This procedure carefully removes the infection from inside the tooth, allowing you to save your natural tooth from extraction. You can learn more about the specific signs you may need a root canal to see if your symptoms line up.
The consequences of ignoring these signs can be severe. According to the World Health Organization's oral health findings, untreated oral diseases are a major global issue, with complete tooth loss affecting about 7% of adults aged 20 and over. This statistic drives home how critical it is to address infections early, before they cause irreversible damage.
Where Dental Infections Start and How They Develop
To understand the danger of a dental infection, it helps to know where the problem begins. These issues usually appear in one of two main areas in your mouth, leading to different kinds of abscesses. Getting a handle on each type is key to understanding why seeing a dentist quickly is so important.
An infection can either start deep inside the tooth itself or get trapped in the gums. While both are serious, knowing the difference can clarify what might be happening and why a dentist would choose a specific treatment.
At the Root of the Problem
The first type is a periapical abscess, which forms at the very tip of a tooth’s root. Think of this as an infection that started inside the tooth—often from an untreated cavity—and traveled down to the end of the root. Bacteria invade the tooth's innermost chamber (the pulp) and spread downwards, creating a painful, pus-filled pocket in the jawbone.
Trapped in a Pocket
The second common type is a periodontal abscess. This happens when an infection gets trapped in the space between your tooth and the gum tissue. This is more of an external issue, often tied to advanced gum disease where deep pockets have formed along the tooth. These pockets are perfect spots for bacteria, food, and plaque to collect, creating the ideal setup for an abscess.
For a closer look at how your gum health plays into these risks, you can learn more about the facts of gum disease and its progression. Understanding that connection is a huge part of prevention.
A dental abscess is actually your body’s way of trying to contain an infection. That collection of pus is a mix of dead white blood cells, tissue debris, and bacteria, forming a barrier to stop the infection from spreading. The problem is, that barrier will eventually fail without treatment.
This infographic breaks down the core signs that often point to one of these infections developing.
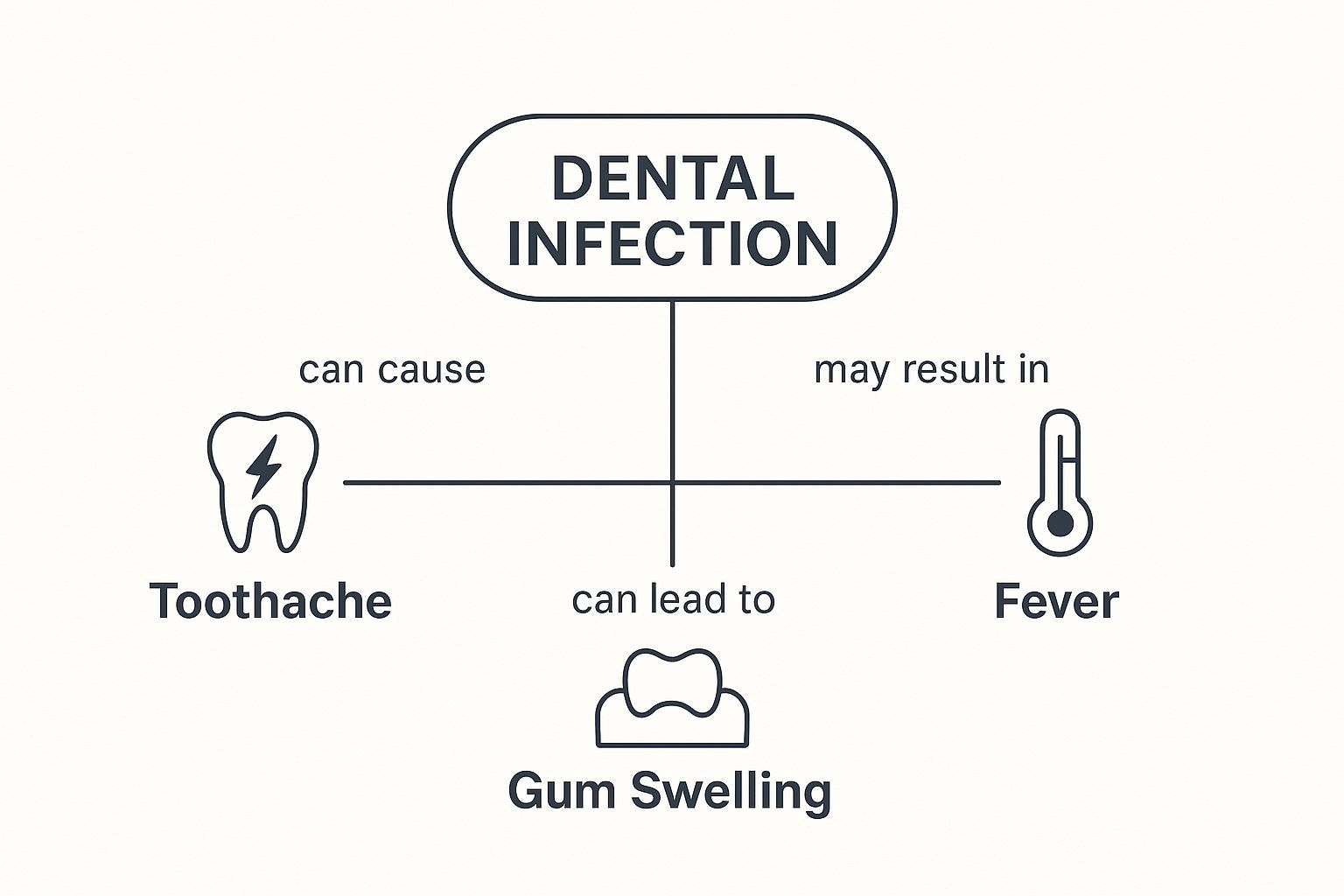
As the visual shows, the central problem of a dental infection leads to some very common and urgent symptoms: tooth pain, gum swelling, and fever. It doesn’t matter if the issue started inside the tooth or in the gums—these warning signs are your body’s alarm system telling you it’s time to get help from your Scottsdale dentist.
Why a Tooth Infection Is a Full-Body Health Risk
It’s a common—and dangerous—mistake to assume a tooth problem stays confined to your mouth. The reality is far more serious. A seemingly localized dental infection is directly connected to your entire body through your bloodstream, posing a significant risk to your systemic health.
Think of an untreated abscess as a launchpad. The bacteria don't just stay put; they can enter your circulatory system and travel to vital areas. This migration can trigger severe secondary infections in your jaw, neck, sinuses, and even your brain.
When the Infection Spreads Systemically
This progression from a local issue to a body-wide crisis is why recognizing the signs of a dental infection is so critical. The most dangerous potential outcome is sepsis, a life-threatening condition where the body’s response to an infection goes into overdrive, causing widespread inflammation.
According to the National Institutes of Health (NIH), sepsis is a medical emergency that can lead to tissue damage, organ failure, and death. It's crucial to understand that what begins as a simple toothache can, in rare but serious cases, escalate into a full-blown systemic crisis.
This highlights the powerful connection between your mouth and your body. Learning how oral health affects your overall wellness is key to understanding why prompt dental care is so important for your long-term health.
Certain symptoms are red flags that the infection has become severe and requires immediate medical attention. Do not wait to seek help if you experience any of the following:
- A high fever, often accompanied by chills.
- Significant facial or neck swelling that makes it hard to fully open your mouth.
- Trouble swallowing or breathing, which is a critical emergency.
These are not "watch and wait" symptoms. They demand an immediate visit to an emergency room or a call to your Scottsdale dentist. This isn't about causing alarm; it's about empowering you to recognize the stakes and make informed decisions for your health.
Common Causes That Open the Door to Infection
Understanding the common culprits that give bacteria an opening is the first step toward keeping your mouth healthy. Think of your teeth like a fortress; certain issues can create a weak spot in the wall, letting harmful bacteria invade.
By far, the most frequent cause is an untreated cavity. When decay is left to its own devices, it eats away at the tooth's protective enamel. This creates a direct tunnel for bacteria to reach the sensitive inner pulp, sparking an infection. But cavities aren't the only way in.
Other common causes include:
- Tiny Cracks: A small, sometimes invisible, crack from grinding your teeth or an old injury is all it takes for bacteria to sneak inside.
- Advanced Gum Disease: As gums pull away from the teeth, they form deep pockets. These pockets are the perfect breeding ground for an infection to take hold.
- Failed Dental Work: Over time, an old filling or crown can become loose or damaged. This allows bacteria to seep underneath and cause trouble all over again.
Lifestyle and Health Factors
Your daily habits and overall health also have a huge say in your risk for infection. A high-sugar diet, persistent dry mouth (which means less protective saliva), or letting your oral hygiene routine slip can put you at a higher risk. This isn't surprising, as oral infections often share risk factors with other health conditions.
The rise in oral diseases is often linked to lifestyle choices, including high sugar consumption, insufficient fluoride, and poor access to dental care. This highlights how integrated your oral health is with your overall wellness.
Once you get a handle on these risk factors, you can start taking real, meaningful steps toward prevention. Learning how to prevent dental problems is an empowering first step in protecting your smile. Recognizing these causes helps you and your Scottsdale dentist build a powerful defense against the signs of dental infection.
How Your Dentist Will Treat the Infection
Once we’ve pinpointed a dental infection, our primary goal is always the same: get rid of the source of the problem, relieve your pain, and stop it from spreading. At Trinity Dental Care, Dr. Fink will walk you through your options with clarity and compassion, making sure you feel completely confident in your treatment plan. The right approach will depend on the type of infection you have and how far it’s progressed.
Thankfully, modern dentistry gives us several highly effective ways to remove an infection and, in many cases, save the tooth. Your treatment will focus on getting to the root cause of the issue, not just covering up the symptoms.
Common Treatment Pathways
The most common treatments for a dental abscess are all about removing the infected tissue while preserving as much of your natural tooth as possible.
Here are the main procedures your dentist might recommend:
- Abscess Drainage: The very first step is often to make a tiny incision in the gum tissue. This allows us to drain the pus from the abscess, providing immediate relief from the intense pressure and pain it causes.
- Root Canal Therapy: If the infection has gotten inside your tooth's pulp, a root canal is the go-to treatment. This procedure involves carefully cleaning out the infected pulp, disinfecting the inner chambers of the tooth, and then sealing it up to prevent reinfection.
- Tooth Extraction: In cases where a tooth is too severely damaged to be saved, an extraction might be the only way forward. Removing the tooth completely eliminates the source of the infection, which is crucial for protecting your overall health.
Antibiotics often play a supportive role in this process. While they can't cure the infection on their own, we prescribe them to control the spread of bacteria and reduce swelling, especially if the infection has started to move into the jaw or other tissues.
Think of it this way: treating the physical source is key. Antibiotics can help fight off the bacterial invaders, but a root canal or extraction removes their home base, ensuring they can’t regroup. Your Scottsdale dentist will create a plan that puts your long-term health first.
When to Call Your Scottsdale Dentist Immediately
Some dental symptoms are more than just uncomfortable—they’re urgent warnings that need a professional’s attention right away. While any persistent pain is a good reason to call us, certain signs point to a serious infection that should not be ignored. Waiting can let the problem get much worse, creating a real risk to your overall health.
Think of these symptoms as your body's emergency alert system. If you experience any of the following, it’s time to act fast.
Urgent Warning Signs
- Severe, throbbing pain that doesn’t go away, even with over-the-counter medication.
- Visible swelling in your gums, cheek, jaw, or even down into your neck.
- A fever, which is a classic signal that your body is fighting a widespread infection.
- Difficulty breathing or swallowing, a critical sign that requires immediate medical care.
- A foul taste in your mouth, which often comes from pus draining from an abscess.
A dental infection will not resolve on its own. While the pain might seem to come and go, the bacteria underneath are still spreading. Without professional treatment, this can lead to severe, body-wide complications.
If you're in Scottsdale and dealing with any of these severe signs, please put your well-being first. This is a dental emergency, and a prompt evaluation is critical. For immediate guidance and care, you can learn more about our emergency dental care services and contact Trinity Dental Care right away.
Your Questions About Dental Infections Answered
When you're dealing with a dental issue, it's natural to have questions. This FAQ section is designed to give you direct, clear answers to the most common questions we hear from our patients in Scottsdale. Our goal is to give you clarity and confidence about what to do next.
1. Can a dental infection go away on its own?
No, a dental infection will not resolve by itself and always requires professional treatment. Sometimes the pain might seem to fade, but that is often a bad sign—it could mean the tooth's nerve has died. The underlying bacteria, however, are still active and will continue to spread, creating a significant risk to your overall health.
2. Will antibiotics alone cure a tooth infection?
Antibiotics are a fantastic tool for getting the spread of bacteria under control and reducing symptoms like swelling, but they cannot cure the infection by themselves. The physical source of the infection—like the decayed tissue inside the tooth—has to be physically removed by a dentist. This is usually done with a procedure like a root canal or by draining the abscess.
3. What is the difference between a gum boil and an abscess?
That small pimple-like bump on your gum, often called a gum boil, is actually the visible sign of a deeper problem—usually a dental abscess. It’s the drainage point for pus that has built up from an infection at the tooth's root. While a canker sore is a shallow ulcer, a gum boil signals a serious infection that needs to be looked at by a dentist right away.
4. How can I manage tooth pain until I see a dentist?
You can take a few steps at home to manage the discomfort temporarily. Remember, these are strictly temporary fixes and are no substitute for seeing a professional.
- Rinse your mouth with warm salt water.
- Apply a cold compress to your cheek to help bring down any swelling.
- Take over-the-counter pain relievers, but only if they are safe for you to use.
It is absolutely critical to see your dentist as soon as possible to treat the cause of the pain.
5. Is a dental infection considered a dental emergency?
Yes, absolutely. Any signs of dental infection—especially if you have severe pain, a fever, swelling in your face, or trouble breathing or swallowing—are a serious dental emergency. These symptoms are red flags that the infection might be spreading. You should contact your Scottsdale dentist immediately for urgent care.
Conclusion: Take Action Against Dental Infections
Recognizing the signs of a dental infection—from persistent pain and swelling to a foul taste or fever—is the first step in protecting your health. These symptoms are your body's way of telling you that something is wrong and requires immediate attention. Ignoring them can lead to serious, system-wide health complications.
Prompt and professional care is the only way to effectively treat a dental infection, relieve pain, and prevent it from spreading. Don't wait for the signs to become a serious health risk. At Trinity Dental Care, Dr. Christine Ann Fink provides compassionate, expert care to patients in Scottsdale, AZ, to resolve your concerns quickly and safely. Contact us today to schedule an appointment by visiting https://trinitydentalcares.com.
