The first signs of gum disease are often so subtle they’re easy to ignore. It usually starts with something as simple as red, swollen, or tender gums that bleed a little when you brush or floss.
You might also notice a nagging bad breath that just won’t go away. These are the classic early warnings of gingivitis, the mildest and most reversible form of gum disease.
Understanding the Silent Threat to Your Smile
Gum disease is sneaky. It often starts without any pain, making it a silent threat that many people in Scottsdale accidentally overlook.
This guide is designed to help you decode what your gums might be trying to tell you. Trinity Dental Care will walk through the journey of gum disease, from the quiet hints of gingivitis to the more serious warnings of periodontitis.
Recognizing these signs early is the single most powerful step you can take to protect your smile. Think of this guide as your resource for spotting potential issues and understanding why professional care is so essential.
The Progression from Healthy Gums to Disease
The path from healthy gums to advanced disease is a clear one. It starts with minor inflammation that can spiral into a serious problem if left unchecked.
This infographic does a great job of showing how gum disease progresses from healthy gums, to gingivitis, and finally to periodontitis.
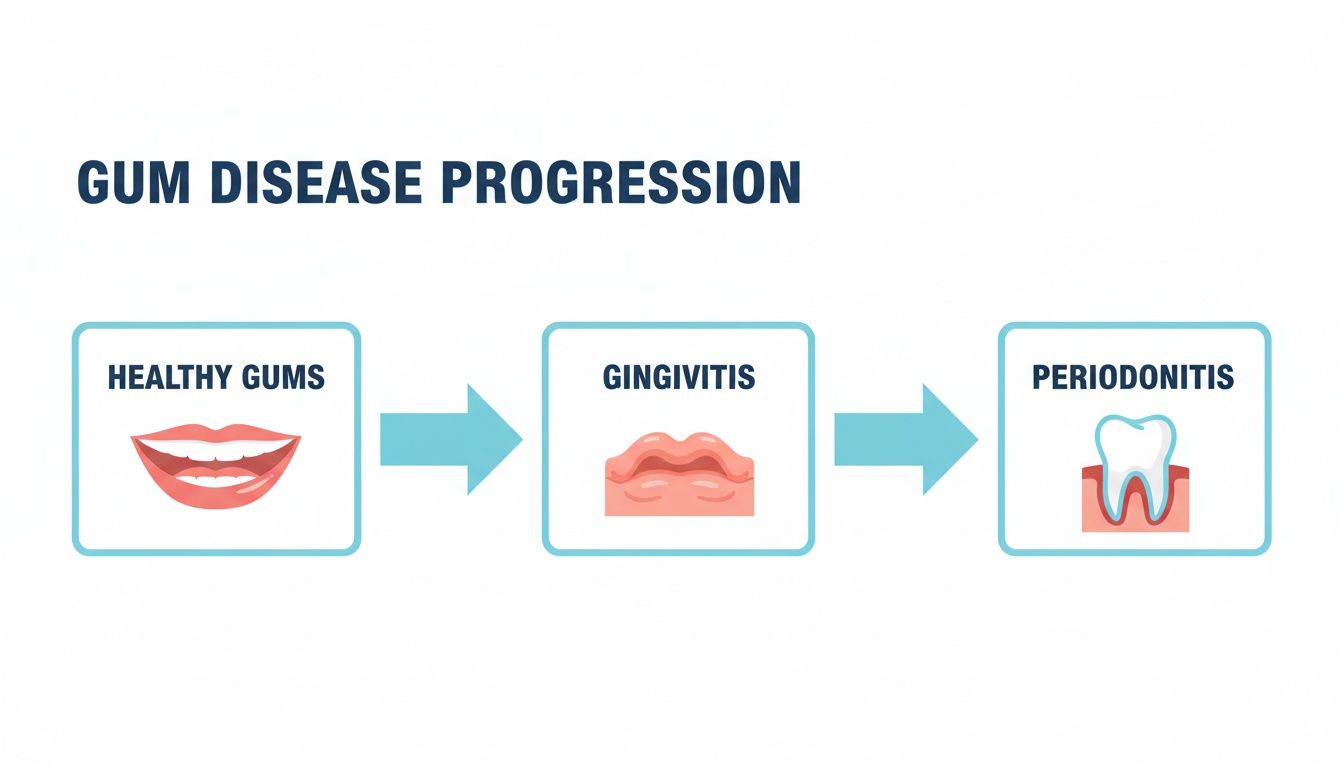
As you can see, the initial stage, gingivitis, is all about inflammation but can often be completely reversed. But without intervention, it can advance to periodontitis, causing irreversible damage to the bone and tissues holding your teeth in place.
Why Early Detection Matters
It’s tempting to dismiss a little pink in the sink as no big deal. But these early warnings are your body’s alarm system.
The bacteria responsible for gum disease don’t just hang out in your mouth. They can slip into the bloodstream, and according to the American Dental Association (ADA), this has been linked to other major health issues.
Understanding how oral health affects your overall wellness is a crucial part of preventive care. The bacteria from inflamed gums can contribute to broader health complications, making proactive dental visits about more than just your teeth.
Taking action the moment you notice symptoms can save you from needing more complex and costly treatments down the road. At Trinity Dental Care, Dr. Christine Ann Fink is passionate about patient education.
Dr. Fink helps Scottsdale residents understand that a healthy mouth is the cornerstone of a healthy life. Addressing the earliest signs of gum disease protects not just your smile, but your entire well-being.
The Early Warning Signs of Gingivitis
Gingivitis is the first chapter in the story of gum disease. Its signs are often so subtle that people brush them off as normal.
But here’s the thing: healthy gums are tough. They’re resilient and should not bleed or look irritated.
Think of your gums as the foundation holding your teeth firmly in place. When harmful bacteria build up along the gumline in that sticky film we call plaque, they start to irritate this sensitive tissue.
Your immune system rushes to the area to fight back, which causes the inflammation, redness, and swelling that define gingivitis. The good news? At this stage, gingivitis is almost always completely reversible.
With a professional cleaning and some simple improvements to your home care, you can get your gums back to perfect health. The key is catching these signs of gum disease early.
1. Pink in the Sink: Bleeding Gums

One of the first things people notice is seeing a little pink or red in the sink after brushing. It’s easy to dismiss this and think, “I must have just brushed too hard.”
But healthy gums can easily handle proper cleaning without bleeding. Bleeding is a direct sign of inflammation, plain and simple.
When plaque sits on your gums for too long, it triggers an immune response. This makes the gum tissue tender and fills it with tiny, fragile blood vessels that break easily.
2. Swollen, Red, or Tender Gums
Healthy gums should have a firm, coral-pink look. When they become puffy, bright red, or even take on a purplish tint, it’s a visible sign of irritation.
This swelling happens because your body is sending more blood to the area. This is an attempt to fight off the bacterial infection brewing along the gumline.
You might also find your gums feel sore or tender to the touch, especially when you’re flossing. This sensitivity is another direct result of that ongoing inflammation.
3. Persistent Bad Breath (Halitosis)
We all get bad breath now and then. But if you have a persistent unpleasant odor that doesn’t go away even after brushing, it could be a symptom of gingivitis.
This condition, known as halitosis, is often caused by the very same bacteria responsible for gum inflammation.
As these bacteria break down tiny food particles trapped between your teeth and gums, they release sulfur compounds. This is what creates that distinct, unpleasant smell.
Oral diseases are incredibly common, affecting an estimated 3.5 billion people worldwide. Understanding these global oral health statistics really highlights why catching these early signs is so crucial.
To help you spot these symptoms at home, here’s a quick self-check guide.
Early Gum Disease Self-Checklist
Use this table as a quick reference to help you identify the most common early symptoms of gingivitis. If you’re noticing one or more of these signs, it’s a good idea to schedule a dental check-up.
| Symptom to Check For | What It Looks Like or Feels Like | Why It Happens |
|---|---|---|
| Bleeding Gums | Seeing pink or red in the sink when brushing or flossing. | Plaque buildup causes inflammation, making gum tissue fragile and prone to bleeding. |
| Redness or Swelling | Gums appear puffy, bright red, or even purplish instead of a healthy pink. | Your body increases blood flow to the gums to fight the bacterial infection. |
| Gum Tenderness | Gums feel sore or sensitive, especially when touched, brushed, or flossed. | Inflammation makes the nerve endings in your gums more sensitive. |
| Persistent Bad Breath | An unpleasant odor that doesn’t disappear with brushing or mouthwash. | Bacteria release smelly sulfur compounds as they break down food debris. |
Improving your daily routine is your first line of defense. You can explore our guide on proper brushing and flossing techniques to make sure your home care is effective.
For our neighbors here in Scottsdale, a professional cleaning at Trinity Dental Care can remove the stubborn tartar that brushing alone can’t. This gives your gums the fresh start they need.
Advanced Signs When Gum Disease Becomes Periodontitis
When the early signs of gingivitis are ignored, the infection digs deeper. It transforms from a reversible annoyance into periodontitis—a far more destructive form of gum disease.
This is where the real damage starts. It moves beyond simple inflammation to actively dismantling the very bone and tissue that hold your teeth in place.
Think of it like a building’s foundation. Gingivitis is like finding a bit of water damage on the drywall; it’s a problem, but you can repair it.
Periodontitis is when that water has seeped into the concrete, slowly eroding the foundation. At this point, the signs of gum disease become much more alarming and signal a clear need for professional help.
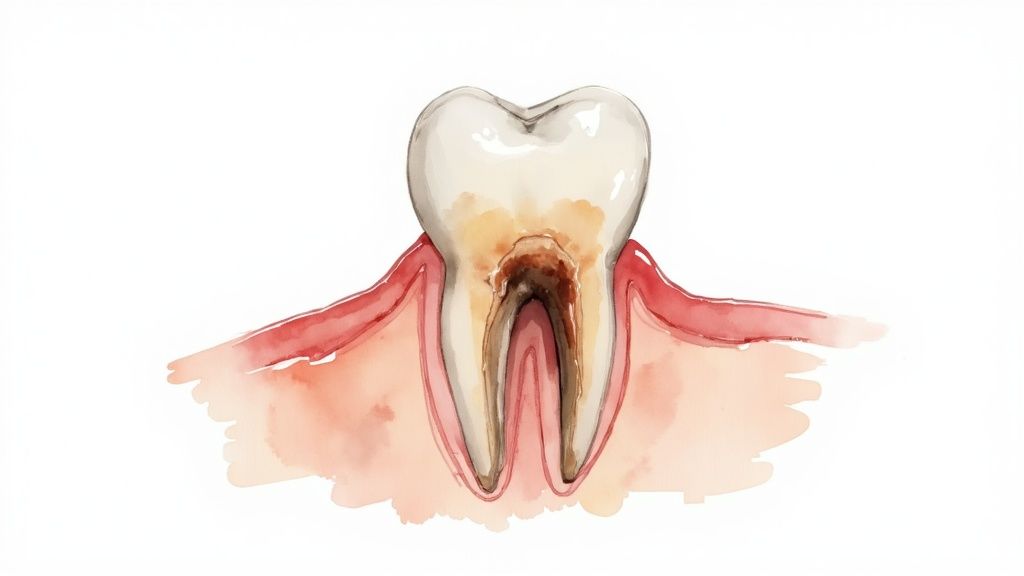
4. Receding Gums and Periodontal Pockets
One of the classic calling cards of periodontitis is gum recession. You might look in the mirror one day and notice your teeth look longer than they used to.
This isn’t your imagination. Your gums are literally pulling away from your teeth, exposing the sensitive root surfaces.
As the gums pull back, they create small gaps called periodontal pockets between the gums and teeth. These pockets are bad news.
They become perfect, shielded breeding grounds for bacteria, safe from your toothbrush and floss. The deeper these pockets get, the more severe the infection.
At Trinity Dental Care, Dr. Christine Ann Fink uses a special probe to gently measure these pocket depths during an exam. A healthy measurement is between 1-3 millimeters. When we see depths of 4 millimeters or more, it’s a clear indicator that periodontitis has set in.
5. Loose Teeth or a Change in Your Bite
This is probably the most unsettling sign of advanced gum disease. If you notice a tooth feels loose or has shifted, it’s a major red flag.
This instability is a direct result of the chronic infection destroying the underlying bone and connective tissues.
You might also feel like your bite has changed. When you close your teeth together, it just feels “off,” or maybe you notice new gaps opening up.
These are all signs that your teeth’s support system is failing. The process of bone deterioration is serious, and learning how to stop bone loss in teeth is critical to preventing tooth loss.
6. Pus Between Teeth and Gums
While early gingivitis is usually painless, periodontitis often brings noticeable discomfort. This shift from a silent problem to a painful one shows how much the disease has escalated.
One alarming symptom is seeing a yellowish-white fluid ooze from your gumline. This is an undeniable sign of a serious infection.
This pus is your body’s attempt to fight off the deep-seated bacteria. It is a clear signal of active destruction happening below your gumline.
7. Pain While Chewing
If it hurts to bite down, it can mean the infection has damaged the ligaments holding your teeth. You may also notice a persistent bad or metallic taste in your mouth.
For those who wear partial dentures, a change in how they fit can also be a symptom of shifting teeth and bone loss.
For Scottsdale residents experiencing any of these symptoms, getting professional care is the most important step you can take. Trinity Dental Care can help stop the damage and protect your overall health.
Key Causes and Personal Risk Factors
Understanding the warning signs of gum disease is a huge first step. But it’s just as important to know why it happens.
The main culprit is always the buildup of bacterial plaque. However, some of us are simply more susceptible than others.
By getting familiar with these risk factors, you can better understand your own health profile. This allows you to work with Dr. Christine Ann Fink to create a proactive plan for protecting your gums.
The Foundation of Gum Disease: Plaque
At its core, gum disease starts with plaque. That is the sticky, fuzzy film of bacteria that’s always trying to form on your teeth.
If you don’t clear it away every day, these bacteria release toxins that irritate your gum tissue. This leads to the inflammation we call gingivitis.
If you let that plaque sit, it hardens into tartar. This is a rough, crusty substance that only a dental professional can remove.
Lifestyle Choices That Increase Your Risk
Some daily habits can dramatically raise your vulnerability to gum disease. These choices can interfere with your body’s ability to fight off infection.
- Tobacco Use: This is one of the biggest ones. It weakens your immune system and reduces blood flow to your gums, making it harder for them to heal.
- Poor Oral Hygiene: Inconsistent brushing and flossing are a direct invitation for plaque to set up camp along your gumline.
- Poor Nutrition: A diet packed with sugar and carbs feeds the bad bacteria in your mouth, while a lack of key nutrients like Vitamin C can weaken your body’s defenses.
Personal Factors You Cannot Control
While you can change your habits, some risk factors are just part of your personal health story. Being aware of them helps you and your dentist stay extra vigilant.
Genetics play a surprising role in oral health. Some individuals are simply more genetically predisposed to developing gum disease, even with diligent home care. This makes regular professional check-ups in Scottsdale even more crucial.
Other inherent risk factors include:
- Hormonal Changes: Fluctuations during puberty, pregnancy, and menopause can make your gums more sensitive and susceptible to inflammation.
- Age: According to the CDC, over 70% of adults 65 and older have some form of periodontal disease.
- Underlying Health Conditions: Diseases that impact the immune system—like diabetes, rheumatoid arthritis, and HIV/AIDS—can lower your body’s resistance to infection.
A recent global study really puts into perspective how widespread this issue has become. Between 1990 and 2021, the incidence of periodontal diseases shot up by over 76%. You can read the full research about these trends to learn more.
How Trinity Dental Care Diagnoses and Treats Gum Disease
Walking into a dental visit worried about your gums can be nerve-wracking. Trinity Dental Care wants to pull back the curtain on the whole process.
Feeling confident and clear about the path forward is the first step toward getting your gums back on track. A gum health evaluation with Dr. Christine Ann Fink is gentle but thorough.
The Diagnostic Process Step by Step
To get the full picture, Trinity Dental Care needs to know what’s going on below the gumline. This next part of the exam is key for figuring out the exact stage of gum disease.
A crucial step involves using a tiny, specialized measuring tool called a periodontal probe. Dr. Fink will gently slide it between your tooth and gum to measure the depth of the pocket.
- Healthy Pockets: In a healthy mouth, these pockets measure between 1 and 3 millimeters.
- Signs of Gingivitis or Periodontitis: Depths of 4 millimeters or more tell us that inflammation has caused the gums to detach from the tooth.
Dental X-rays may also be taken to check for any bone loss around your teeth. This is a tell-tale sign of advanced periodontitis.
Your Path to Healthier Gums: Treatment Options
Once a diagnosis is made, the goal is to stop the disease in its tracks. The treatment recommended will depend entirely on how severe the infection has become.
The most common treatment for active gum disease is scaling and root planing, often referred to as a “deep cleaning.” This procedure is designed to meticulously remove plaque and hardened tartar from both above and below the gumline.
This process involves two main steps:
- Scaling: Carefully clearing away all the plaque and tartar buildup from your tooth surfaces.
- Root Planing: After scaling, the tooth roots are smoothed out. This helps your gums reattach firmly to your teeth.
This treatment is the cornerstone for halting the progression of gum disease. You can learn more about what a deep cleaning is and why it’s so effective.
Your Partner for Healthy Gums in Scottsdale
Facing concerns about your gum health can feel overwhelming, but you don’t have to navigate it alone. Trinity Dental Care is your dedicated partner in Scottsdale.
Dr. Christine Ann Fink’s patient-first philosophy means combining modern technology with genuine empathy. The goal is to ensure you feel comfortable, informed, and truly cared for.
Ignoring the early signs of gum disease is a gamble. It can open the door to far more serious health issues down the road.
Severe periodontitis isn’t a small issue—it’s a global problem affecting over 1 billion people worldwide as of 2021. The consequences, like tooth loss, are only expected to become more common. You can learn more about the global impact of gum disease to see just how critical proactive care is.
“A healthy smile is built on a foundation of healthy gums. We believe in empowering our patients with the knowledge and care they need to protect that foundation for a lifetime.”
– Dr. Christine Ann Fink, Trinity Dental Care
If you have any concerns about your gums, please don’t wait for the symptoms to get worse. Our specialized periodontal care in Scottsdale is designed to halt gum disease.
Answers to Your Top Questions About Gum Disease
When it comes to gum health, it’s natural to have a lot of questions. Here are the most common concerns Trinity Dental Care hears from patients in Scottsdale.
1. Can gum disease be cured permanently?
The good news is that gingivitis, the earliest stage, is almost always completely reversible. A professional cleaning at Trinity Dental Care and solid home care are usually all it takes.
However, once the disease advances to periodontitis, the goal shifts from “cure” to “management.” The damage to the bone and supporting tissues is permanent, so our focus is on stopping the disease and maintaining your oral health.
2. Is it normal for gums to bleed when I floss?
It might be common, but it is absolutely not normal. Healthy gums are firm and resilient and shouldn’t bleed from gentle brushing or flossing.
Bleeding is an alarm bell and one of the most classic early signs of gum disease. It’s a signal that inflammation is present due to plaque buildup.
3. How is gum disease linked to other health problems?
The connection between your mouth and body is incredibly strong. The chronic inflammation from gum disease doesn’t just stay put.
Bacteria can enter your bloodstream, traveling throughout your body and contributing to serious health issues. We now know there are significant links between periodontitis and conditions like heart disease, stroke, and trouble managing diabetes.
4. What is the difference between a regular and deep cleaning?
A regular cleaning, or prophylaxis, is a preventive measure. It’s designed for a healthy mouth to remove plaque and tartar from above the gumline.
A deep cleaning, or scaling and root planing, is a therapeutic treatment for active gum disease. This procedure goes below the gumline to remove hardened tartar from tooth roots inside periodontal pockets.
5. Can I treat gum disease at home without a dentist?
Excellent home care is your most important line of defense. Diligent brushing and daily flossing are absolutely essential for managing plaque day-to-day.
However, home care alone cannot treat active gum disease. Once plaque hardens into tartar, it can only be removed by a dental professional with specialized tools.
Ready to protect your smile with expert care in Scottsdale? Contact Trinity Dental Care today to schedule a personalized consultation with Dr. Christine Ann Fink. Schedule your personalized consultation today and take the first step toward healthier gums.
