Worried about your gums? It’s easy to overlook the earliest signs of gum disease, like seeing a little pink in the sink when you brush or having gums that look redder and more swollen than usual. You might even have persistent bad breath that mouthwash just can't seem to fix.
These aren't just minor annoyances; they're your body's first warning signals. Ignoring them can lead to more serious issues down the line.
Your Guide to Understanding Gum Health

Gum disease is a sneaky condition that affects millions of people, often without them even realizing it. Many Scottsdale, AZ, residents might not notice anything is wrong until the problem has quietly progressed. Trinity Dental Care knows that understanding the first whispers of trouble is your best defense.
This guide is for anyone who wants to be proactive about their oral health. Think of your gums as the foundation holding your teeth firmly in place; if that foundation weakens, the whole structure is at risk. We'll walk through everything from the mild stage, gingivitis, to the more serious condition, periodontitis.
What Is Gum Disease?
At its core, gum disease—or periodontal disease—is an infection of the tissues that support your teeth. It all starts with plaque, that sticky, fuzzy film of bacteria that builds up on your teeth every day. When brushing and flossing don't clear it away, it hardens into tartar, and your immune system jumps into action, causing inflammation.
That initial stage, gingivitis, is what you see when your gums get puffy, red, and tender. The great news? Gingivitis is completely reversible with a professional cleaning and a little extra attention to your home care routine. But if it's ignored, that inflammation doesn't just go away.
Why Early Detection Matters
Letting those early signs slide allows gingivitis to advance into periodontitis, which is where things get serious. The infection moves below the gumline, creating pockets and starting to break down the bone and connective tissue that anchor your teeth. This damage is permanent and can ultimately lead to loose teeth and even tooth loss.
Catching the symptoms early is everything. Think of it as your body's check-engine light coming on—it's signaling that it's time for a professional to take a look. A solid understanding of how to maintain healthy gums and why it's important is the first step toward lifelong dental wellness.
As Dr. Christine Ann Fink always says, an informed patient is an empowered patient. This guide will give you the knowledge you need to protect your smile for a lifetime.
Spotting the Early Warning Signs of Gingivitis
Gingivitis is the very first stage of gum disease, and its symptoms are often so subtle they're easy to brush off. Think of it as a quiet heads-up from your body that something isn’t quite right. Ignoring it is like ignoring the "check engine" light in your car—the issue is small now but can lead to bigger problems.
The good news? At this stage, gum disease is 100% reversible. With a professional cleaning from a trusted Scottsdale dentist like Dr. Christine Ann Fink and more diligence at home, you can stop the inflammation completely. Recognizing the early signs is the critical first step.
Seeing Pink in the Sink: Bleeding Gums
One of the most common signs of gum disease is seeing a bit of blood after you brush or floss. Healthy gums are surprisingly tough and shouldn't bleed from routine cleaning. That bleeding is happening because plaque has built up along your gumline, irritating the delicate tissue and making it inflamed.
Many people mistakenly think that seeing blood means they should brush less, but the opposite is true. It’s a clear signal that plaque is accumulating where it shouldn't be. You can brush up on the right way to clean your teeth with our guide on proper brushing and flossing techniques.
Puffy, Swollen, and Red Gums
Healthy gums should look firm and coral-pink, fitting snugly around your teeth. When gingivitis starts to take hold, that picture changes. You might notice your gums look puffy, swollen, or have taken on a reddish or even purplish tint.
This is your body’s inflammatory response to the bacterial toxins in plaque. That swelling can also make your gums feel tender to the touch, especially when you're brushing.
According to the CDC, nearly half of adults aged 30 and older have some form of periodontal disease. This prevalence intensifies with age, with nearly 70% of seniors aged 65 and above showing signs of periodontal issues.
Healthy Gums vs. Early Gingivitis: A Visual Guide
Sometimes, a side-by-side comparison makes it easier to spot a problem. Use this quick guide to assess your own gum health and see if it’s time to schedule a visit with Dr. Christine Ann Fink at Trinity Dental Care.
| Symptom | Healthy Gums | Signs of Gingivitis |
|---|---|---|
| Color | Consistently pale, coral-pink | Red, dark red, or even purplish |
| Texture | Firm and resilient to the touch | Soft, puffy, and swollen |
| Bleeding | Does not bleed during brushing or flossing | Often bleeds easily with minor contact |
| Shape | Fits snugly and tightly around each tooth | May look pulled back or puffy around teeth |
By paying attention to these early warnings, you give yourself the power to act fast. Catching gingivitis at this stage is the key to preventing irreversible damage and keeping your smile healthy for years to come here in Scottsdale.
Recognizing the Advanced Signs of Periodontitis
When the early signs of gingivitis are ignored, that bacterial infection digs deeper, escalating into a far more serious condition called periodontitis. This is the advanced stage of gum disease, where permanent, irreversible damage starts to set in.
Unlike gingivitis, periodontitis is a full-blown attack on the underlying structures that hold your teeth in place. Your body's own immune system, trying to fight the chronic infection, actually starts breaking down the bone and connective tissues. This destructive process kicks off a series of alarming symptoms you should never overlook.
Gums Pulling Away From Your Teeth
One of the most obvious advanced signs of gum disease is seeing your gums recede. You might look in the mirror one day and think your teeth suddenly look longer than they used to. This isn't your imagination—it's the direct result of your gum tissue physically pulling away from the tooth surface.
This recession exposes the sensitive root of the tooth, which can make eating or drinking anything hot or cold painful. More importantly, it’s a red flag that the gums are detaching from the teeth. As the gums pull away, they create deep pockets where more harmful bacteria can hide and accelerate the damage.
The Formation of Deep Pockets
As your gums recede, the space between the gum tissue and the tooth deepens, forming what dentists call periodontal pockets. In a healthy mouth, this gap is very shallow, usually between 1 to 3 millimeters deep. When periodontitis takes hold, these pockets can deepen to 4, 5, or even more millimeters.
These pockets are impossible to clean with regular brushing and flossing, trapping food debris and allowing bacteria to multiply. This creates a vicious cycle of infection that continuously eats away at the bone supporting your teeth. At Trinity Dental Care, Dr. Christine Ann Fink uses a special tool to gently measure these pocket depths—a key part of diagnosing the disease's severity.
Periodontitis is a significant global health issue. As of 2021, over 1 billion people worldwide were living with a severe form of the disease. This condition is a leading cause of tooth loss and is projected to affect an estimated 1.56 billion individuals by 2050. You can explore more about the global impact of gum disease and its prevalence in recent studies.
Changes in Your Bite and Tooth Alignment
As periodontitis destroys the jawbone, the very foundation holding your teeth in place becomes weak and compromised. The consequences of this bone loss aren’t just happening out of sight; they become physically noticeable.
You might start to experience one or more of these major red flags:
- Loose or Shifting Teeth: Your teeth might feel wobbly. This is a direct sign that a significant amount of bone support has already been lost.
- New Gaps Forming: You could notice new spaces appearing between your teeth where none existed before as they begin to drift.
- Changes in Your Bite: When you bite down, your top and bottom teeth may not fit together the way they always have.
These are unmistakable signs that the disease is actively destroying your jaw. It’s crucial to address the root cause of this destruction. You can learn more about how to stop bone loss in teeth in our detailed guide.
Understanding the Root Cause of Gum Disease
To understand the signs of gum disease, it helps to know what's causing the trouble. The main culprit is plaque, a sticky, colorless film of bacteria that’s constantly forming on your teeth. It’s that fuzzy coating you might feel when you first wake up.
When you don't clear away plaque every day with good brushing and flossing, it hardens into tartar, or calculus. Tartar is like cement for bacteria; once it forms, your toothbrush can't remove it. It latches onto your tooth surface, especially along and just below the gumline.
From Plaque to Tartar: The Vicious Cycle
Tartar creates a rough, porous surface that’s a perfect breeding ground for even more plaque and bacteria to pile on. This buildup becomes a constant source of irritation for your gums.
The bacteria thriving in plaque and tartar release toxins, and your body’s immune system responds by kicking off an inflammatory reaction. This initial inflammation is gingivitis—the earliest and most reversible stage of gum disease. At this point, your gums get red and swollen, but the bone and tissues holding your teeth are still safe.
When Inflammation Turns Destructive
If gingivitis isn't addressed, that inflammation becomes chronic. This is where things take a more dangerous turn. Your body's immune system starts attacking not just the bacteria but also the very tissues and bone that support your teeth.
This destructive phase is known as periodontitis. What makes this process so deceptive is that it's often silent and painless in its early stages. The infographic below shows how this damage progresses from simple gum recession all the way to bone loss.
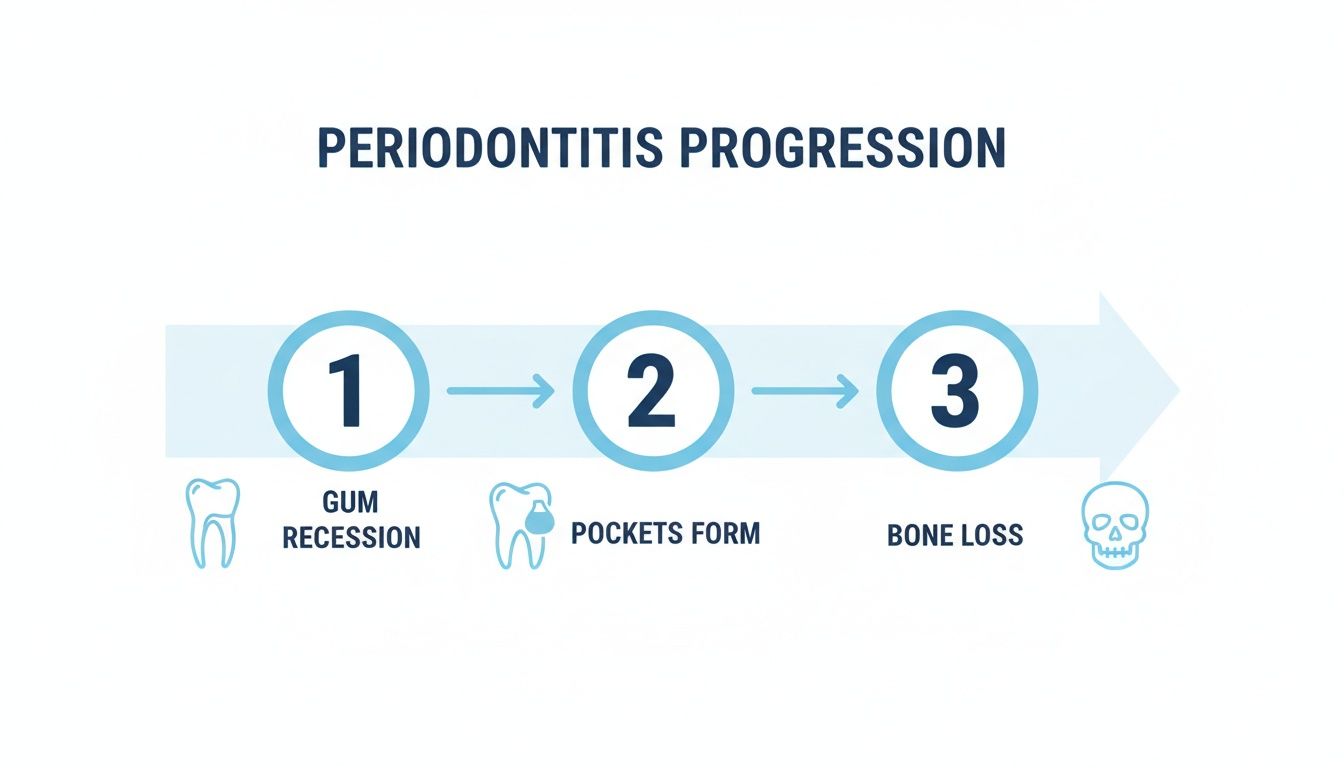
As the visualization shows, the journey from healthy gums to advanced periodontitis is a step-by-step breakdown of your smile's very foundation, which can ultimately lead to tooth loss if it isn't stopped.
Risk Factors That Increase Your Susceptibility
While plaque is always the primary cause, certain factors can make some people more vulnerable to developing gum disease. These risk factors can speed up the disease's progression or make it tougher to treat.
Your body's response to the chronic inflammation of gum disease is the real source of damage. The immune system's attempt to fight the infection ends up destroying the bone and tissues crucial for holding your teeth securely.
Understanding these influences is key to taking a proactive approach. Dr. Christine Ann Fink always considers a patient's complete health profile when diagnosing and treating gum disease at Trinity Dental Care.
Key risk factors include:
- Smoking & Tobacco Use: This is one of the most significant risk factors. It weakens your immune system, making it harder for gums to heal.
- Genetics: Unfortunately, some people are simply more genetically predisposed to gum disease.
- Diabetes: People with diabetes are at a higher risk for developing infections like gum disease.
- Hormonal Changes: Shifts in hormones during puberty, pregnancy, and menopause can make gums more sensitive.
- Certain Medications: Some drugs can reduce saliva flow, leading to a dry mouth that allows plaque to build up more easily.
How We Diagnose and Treat Gum Disease in Scottsdale
Recognizing the signs of gum disease is a crucial first step, but a professional diagnosis is where the path to healing begins. At Trinity Dental Care, our process is clear, thorough, and comfortable, giving Scottsdale residents a personalized plan to stop the disease.
What’s happening below the gumline is often the most important part of the story. That’s why Dr. Christine Ann Fink combines a careful visual examination with precise diagnostic tools to get the complete picture.
Your Comprehensive Gum Health Evaluation
Your journey back to health starts with a detailed evaluation. This isn’t just a quick look—it’s a systematic assessment where Dr. Fink performs checks to determine the stage and severity of any gum inflammation or infection.
This evaluation typically includes:
- Measuring Periodontal Pockets: Using a small, specialized ruler, Dr. Fink gently measures the depth of the space between your teeth and gums.
- Checking for Bleeding Points: Gentle probing helps identify areas where gums are inflamed and bleed easily, a classic sign of active infection.
- Assessing Gum Recession: We carefully document any areas where the gums have started to pull away from the teeth.
- Evaluating Tooth Mobility: We check for any looseness in your teeth, which can be a sign of advanced bone loss.
Looking Beneath the Surface with Digital X-Rays
Some of the most significant damage from gum disease happens completely out of sight. Digital X-rays are an essential tool that allows Dr. Fink to see what’s going on with the bone that supports your teeth. This technology gives us a clear view of your jawbone, revealing any bone loss that has occurred.
The global impact of periodontal diseases is staggering. In 2021 alone, there were approximately 89.6 million new cases reported, with the total number of people affected exceeding 1 billion. You can learn more about these global oral health trends to see why early intervention is so important.
Personalized Treatment Plans Starting with Non-Surgical Options
Once we have a clear diagnosis, we create a personalized treatment plan. For most patients with early-to-moderate gum disease, our first line of defense is a non-surgical treatment known as scaling and root planing.
At Trinity Dental Care, our primary goal is to halt the progression of gum disease comfortably and effectively. We focus on non-surgical treatments first to restore your oral health with the most conservative approach possible.
Scaling and root planing is essentially a deep cleaning that goes where a regular cleaning can’t. You can explore what is a deep cleaning in more detail in our dedicated guide.
The process involves two main steps:
- Scaling: Dr. Fink carefully removes all the plaque and hardened tartar from both above and below the gumline.
- Root Planing: After the tartar is gone, the tooth roots are gently smoothed to help prevent new bacteria from sticking.
This thorough cleaning removes the bacterial irritants, allowing the inflammation to subside so your gums can begin to heal. At Trinity Dental Care, we are committed to helping our Scottsdale patients regain control of their oral health.
Common Questions About Gum Disease Answered
Navigating dental health can bring up a lot of questions. Dr. Christine Ann Fink and the Trinity Dental Care team believe in patient education, because clear answers lead to better health. We've gathered the most common questions our Scottsdale patients ask.
Can Gum Disease Be Completely Cured?
This is one of the most frequent questions we hear, and the answer depends on the stage.
- Gingivitis: Yes, absolutely. Gingivitis, the earliest stage, is fully reversible with a professional cleaning and solid home care.
- Periodontitis: Once gum disease advances to periodontitis, the damage done to bone and gum tissue is permanent. The good news is that we can successfully manage it to stop it from getting worse.
Are Bleeding Gums Normal When I Floss?
Absolutely not. Bleeding gums are never normal and should always be treated as a major warning sign. It's one of the most common early signs of gum disease.
If you consistently see blood on your floss, it’s a clear signal that plaque is causing inflammation. Don't stop flossing—that's your cue to be even more diligent and to schedule a check-up with us.
How Does Gum Disease Affect My Overall Health?
The link between your mouth and the rest of your body is incredibly strong. Gum disease isn't just a "mouth problem"; it's a chronic inflammatory condition that can have serious ripple effects.
The bacteria and inflammation from infected gums can sneak into your bloodstream and travel throughout your body. This can contribute to or even worsen other major health issues.
There is a strong, scientifically-proven link between gum disease and systemic health issues like heart disease and diabetes. Taking care of your gums is a crucial part of taking care of your total health.
The chronic inflammation with periodontitis can directly impact your cardiovascular system. Understanding how bad teeth can affect your heart is key to grasping the full picture.
What Is a Deep Cleaning?
A standard cleaning focuses on removing plaque and tartar from above the gumline. A deep cleaning, or scaling and root planing, is a specific treatment for active gum disease.
The process has two main steps:
- Scaling: We carefully remove plaque and hardened tartar from your teeth, both above and below the gumline.
- Root Planing: We smooth out the roots of your teeth to help your gums heal and reattach firmly.
What Should I Do If I See Signs of Gum Disease?
If you notice any of the signs of gum disease—from bleeding gums to loose teeth—the single most important thing you can do is schedule a dental appointment right away. Don't wait hoping it will go away on its own.
Early action is the best way to prevent severe, permanent damage. Here in Scottsdale, Dr. Christine Ann Fink can give you an accurate diagnosis and create a personalized treatment plan to get your oral health back on track.
Your smile deserves the best care. If you're concerned about your gum health or have noticed any potential signs of gum disease, don't wait. The team at Trinity Dental Care is here to provide the expert diagnosis and compassionate treatment you need.
Ready to take the next step toward healthier gums in Scottsdale? Contact Trinity Dental Care today to schedule a personalized consultation with Dr. Christine Ann Fink.
